 Patients with a score of 3 to 4 were screened according to the TIMI (Thrombolysis in Myocardial Infarction) score 11. We obtained information on the study population from the Chinese Acute Myocardial Infarction Registry, and after considering the completeness of the information, we selected all patients with NSTE-ACS from November 2014 to January 2017.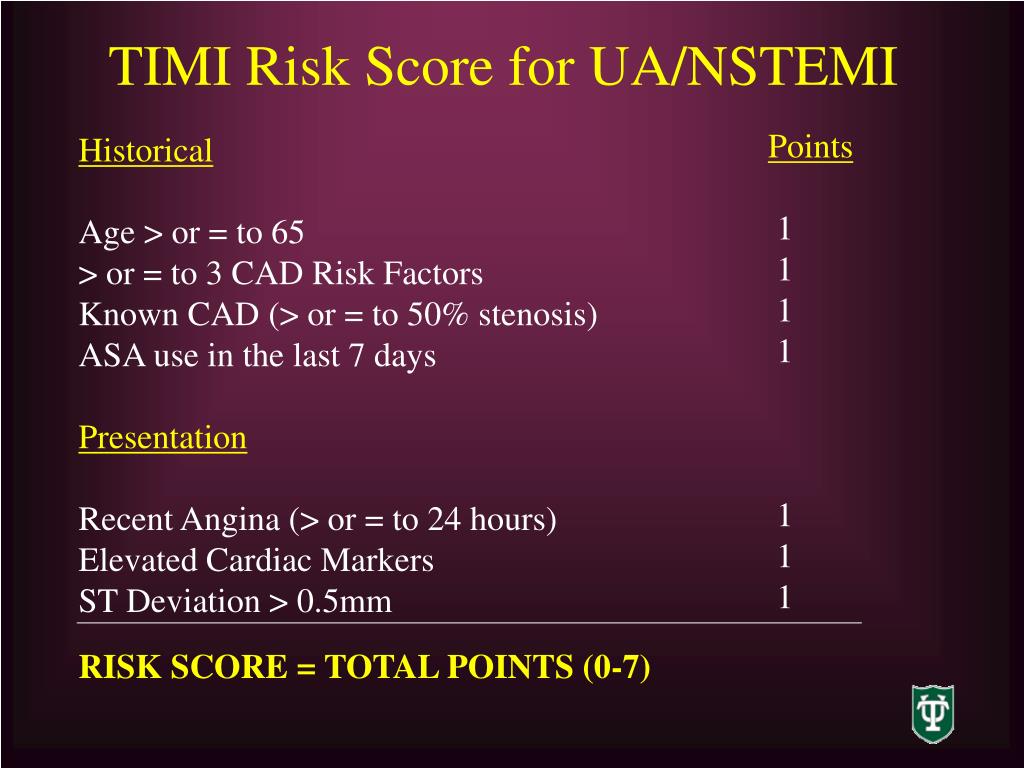 
All methods were performed in accordance with the relevant guidelines and regulations. The study design and methodological specifics of the project have been published 10. This study was jointly initiated by the American Heart Association and the Chinese Society of Cardiology in 2014. The CCC-ACS project is a nationwide registry and quality improvement study with a constantly updated database placing emphasis on ACS care. Then, we reviewed their in-hospital clinical outcomes. Thereafter, we grouped patients according to the time interval from the onset of cardiac symptoms to PCI. The primary purpose of our study was to first select intermediate-risk NSTE-ACS patients. Additionally, based on the data in the CCC (Improving Care for Cardiovascular Disease in China), we decided to analyze the prognosis according to the timing of PCI in patients with intermediate-risk NSTE-ACS in China. Current studies have shown no significant difference between early invasive treatment and immediate invasive or delayed invasive approaches, but these studies often start at the time of admission, which may lead to significant heterogeneity in the trial cohort in terms of timing intervals, so we planned the starting point of this study to be at the onset of symptoms to reduce the impact of such issues 7, 8, 9. However, the optimal timing of this intervention for intermediate-risk patients has not been well defined. As a result, the latest guidelines from the American College of Cardiology-American Heart Association and the European Society of Cardiology recommended that an early invasive approach should be performed within 24 h in high-risk NSTE-ACS patients and within 72 h in intermediate-risk NSTE-ACS patients 5, 6. An early invasive strategy of coronary angiography was favored, especially in high-risk subgroups, and this strategy has been shown to be beneficial in many studies 3, 4. 
A routine early invasive strategy of early angiography followed by revascularization was compared with a conservative strategy of angiography and subsequent revascularization, which was performed only in patients in whom drug therapy failed or those with substantial residual ischemia. Patients with NSTE-ACS are at risk for adverse cardiac events because of refractory angina and hemodynamic or electrical instability 2, 3. Therefore, we need to pay more attention to what is relevant in the context of follow-up treatment. Currently, the incidence of non-ST-elevation acute coronary syndrome is almost twice that of ST-elevation acute coronary syndrome 1. Percutaneous coronary intervention (PCI) treatment is still the main treatment option. The pain that occurs in acute coronary syndrome is often caused by thrombus obstruction, and the thrombus that appears when myocardial infarction occurs is currently considered to be a white thrombus, with platelets as the main component, which does not allow thrombolysis to solve the problem. 
Non-ST-elevation acute coronary syndrome (NSTE-ACS) is a specific type of acute coronary syndrome that often presents with ischemic chest pain but does not show typical ST-segment elevation on electrocardiogram. The incidence of in-hospital MACEs among patients who underwent revascularization within 48 h is lower than that of patients who underwent revascularization after 48 h. The results of revascularization within 48 h were similar, and the incidence of in-hospital MACEs was lower than when revascularization was completed after 48 h. The results of the chi-square test showed that there was a significant difference in the incidence of in-hospital major adverse cardiovascular events (MACEs) when revascularization was completed within 48 h than when it was completed after 48 h (P < 0.05). Risk factors, management and in-hospital outcomes were analyzed in the four groups. A total of 2835 patients with intermediate-risk NSTE-ACS (TIMI score 3–4) included in the China Acute Myocardial Infarction Registry from November 2014 to January 2017 were analyzed according to the time window from symptom onset to revascularization: within 24 h, Group I (814/28.7%) within 24 to 48 h, Group II (526/18.6%) within 48 to 72 h, Group III (403/14.2%) and after 72 h, Group IV (1092/38.5%). There was uncertainty about the routine revascularization time in patients with intermediate-risk NSTE-ACS. We applied the Thrombolysis in Myocardial Infarction (TIMI) score for risk stratification of patient prognosis. Non-ST-elevation acute coronary syndrome (NSTE-ACS) is a specific type of acute coronary syndrome. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
